Tuberculous Atlanto-axial dislocation – How to manage?
|
|
Tuberculous Atlanto-axial dislocation – How to manage?
02/10/2023
02/10/2023
https://www.pediatriconcall.com/Journal/images/journal_cover.jpg
Suhani Jain1, Ira Shah2.
1Grant Government Medical College, Sir JJ Group of Hospitals, Mumbai, India,
2Consultant in Pediatric Infectious Diseases, Levioza Health Care, Mumbai, India.
ADDRESS FOR CORRESPONDENCE
Suhani Jain, Flat number 402, Ramdeo Arise, Behind Hotel Airport Centre Pt, Wardha Road, Nagpur-440025.
Email: suhani2208@gmail.com
Pediatric Tuberculosis, atlanto-axial dislocation, TB spondylitis
|
Clinical Problem
An 8-year-old girl presented with pain and inability to extend her neck for three months. She had a history of occasional low-grade fever during this period, but she was afebrile at presentation. There had been no prior trauma or surgery. There was no history of contact with a patient suffering from tuberculosis (TB). On examination, weight was 24 kg(at 50th centile as per Indian Academy of Paediatrics (IAP) 2015 growth charts), height was 125 cms (at 50th centile as per IAP 2015 growth charts) and Body mass Index (BMI) was 15.4 kg/m2.(between 50th and overweight percentile as per IAP 2015 growth chart).
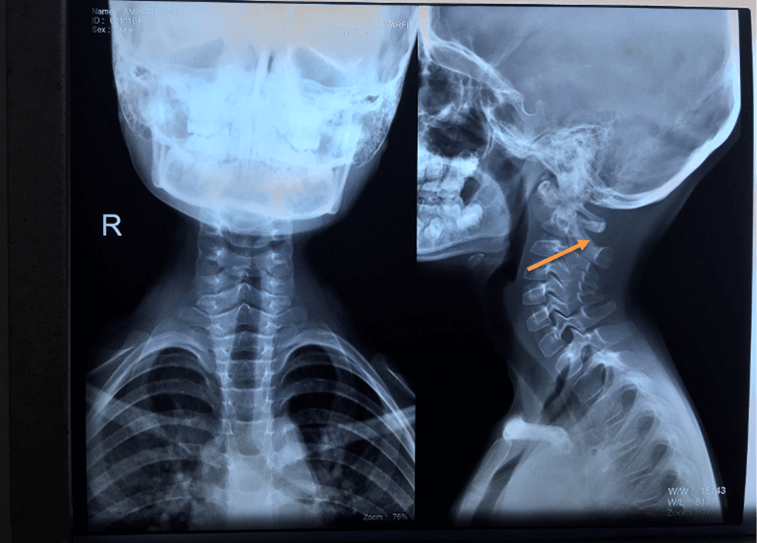
There was restriction in extension of the neck with pain but there was no swelling. Other general examination and systemic examination were normal. There was no neurological deficit. X-ray of the cervical spine showed dislocation of the atlanto-axial joint (Figure 1). MRI cervical spine showed a lytic lesion with associated granulation tissue in the left lateral mass of the atlas bone. This granulation tissue appeared to be extending into the atlanto-dental interspace. There was atlantoaxial dislocation and mild indentation of the cervicomedullary junction by the odontoid process and there was no evidence of cord edema or myelomalacia, thus suggestive of tuberculosis (TB). Mantoux test by 5 TU PPD-S was positive (10 mm). Chest X-ray was normal.
Figure 1. X-ray of the cervical spine showing dislocation of the atlanto-axial joint.
|
| |
How to manage this patient further?
|
|
|
Discussion
Atlantooccipital dislocation, a condition characterized by the misalignment of the uppermost spinal bones, can arise from various causes such as congenital factors, trauma or inflammation.1 In the case of our patient, the absence of any traumatic history is notable. Instead, the presence of a positive Mantoux test and clinical manifestations including long-standing fever, coupled with the appearance of granulation tissue extending into the atlanto-dental interspace, suggests an infective etiology like TB.
TB spondylitis affects 1% of TB patients. Atlantoaxial involvement is exceptionally uncommon, accounting for 0.3%-1% of TB spondylitis cases.2 Atlantoaxial TB can cause joint instability due to the destruction of the atlantoaxis ligament and bone, resulting in neck pain, torticollis, neurologic impairment and even sudden death.3
Three different approaches can be used to treat atlantoaxial TB: conservative treatment, surgical treatment and a mixed approach based on radiologic findings and clinical symptoms, which is preferred by more surgeons.3
According to Kalra et al, the goal of surgery is tissue diagnosis, relieve neural compression (if any) and stabilise the patient.4 Conservative treatment is usually accepted by patients who do not have neurologic symptoms or atlantoaxial instability. Treatment for patients with neurologic impairment and atlantoaxial instability, on the other hand, is debatable.3
In this patient, there is C1-C2 involvement with dislocation, but there are no neurological deficits which is why we could go for conservative treatment and not a surgical approach. Surgical reduction and fixation carry risk like injury to the Vertebral artery which has proven to have dangerous complications like exsanguination or other serious injuries.1 A Conservative approach would involve cervical traction for initial 3 months followed by a brace along with multidrug antitubercular drugs.5 In our patient, we started first line antitubercular therapy (ATT) consisting of isoniazid (H), rifampicin (R), pyrazinamide (Z) and ethambutol (E) for 2 months followed by 10 months of HRE based on clinically diagnosed TB and did not go for surgical intervention or biopsy due to risk of complications.He was also given a cervical brace for the dislocation. It has been advised that in cases of spinal tuberculosis with evidence of cord compression and severe neurological compromise, steroids can be used in adjunction with ATT regimen.6
Our patient was not started on steroids as there was no neurological deficit. He was subsequently lost to follow-up.
|
| |
| Compliance with ethical standards |
|
Funding: None
|
|
|
Conflict of Interest: None
|
- Yang SY, Boniello AJ, Poorman CE, Chang AL, Wang S, Passias PG. A review of the diagnosis and treatment of atlantoaxial dislocations. Global Spine J. 2014 Aug;4(3):197-210. doi: 10.1055/s-0034-1376371. Epub 2014 May 22. PMID: 25083363; PMCID: PMC4111952.. [CrossRef] [PubMed] [PMC free article]
- Sridharan S, Arumugam T. Atlantoaxial tuberculosis: Outcome analysis. Int J Mycobacteriol. 2017 Apr-Jun;6(2):127-131. doi: 10.4103/ijmy.ijmy_55_17. PMID: 28559512. [CrossRef] [PubMed]
- Bao D, Li L, Gong M, Xiang Z. Treatment of Atlantoaxial Tuberculosis with Neurological Impairment: A Systematic Review. World Neurosurg. 2020 Mar;135:7-13. doi: 10.1016/j.wneu.2019.09.073. Epub 2019 Sep 21. PMID: 31550536. [CrossRef] [PubMed]
- Kalra SK, Kumar R, Mahapatra AK. Tubercular atlantoaxial dislocation in children: an institutional experience. J Neurosurg. 2007 Aug;107(2 Suppl):111-8. doi: 10.3171/PED-07/08/111. PMID: 18459882. [CrossRef] [PubMed]
- Chadha M, Agarwal A, Singh AP. Craniovertebral tuberculosis: a retrospective review of 13 cases managed conservatively. Spine (Phila Pa 1976). 2007 Jul 1;32(15):1629-34. doi: 10.1097/BRS.0b013e318074d41e. PMID: 17621210. [CrossRef] [PubMed]
- Cruz IE, Ferreira P, Machado SB, Torres JM, Miranda C, Antunes I. Spinal Tuberculosis - Treatment Options Beyond Guidelines. Ann Clin Case Rep. 2019; 4: 1776. [CrossRef]
|
|
| |
Cite this article as:
Jain S, Shah I. Tuberculous Atlanto-axial dislocation – How to manage?. Pediatr Oncall J. 2023;20: 164-165. doi: 10.7199/ped.oncall.2023.54
|