Caroline Lopes1, Cristina Amaro2
1General Pediatric Department, Hospital de Santo André - Centro Hospitalar de Leiria, EPE, Leiria, Portugal, 2Dermatology Department, Hospital de Egas Moniz - Centro Hospitalar de Lisboa Ocidental, Lisboa, Portugal
Address for Correspondence: Caroline Lopes, Hospital de Santo André, R. de Santo André, 2410-197 Leiria.
Email: reislopescaroline@hotmail.com
|
Question :A healthy 8-year-old boy was observed in a Dermatology consultation, with a 4-week history of an erythematous patch on the scalp with alopecia measuring approximately 3 cm long axis. Scalp dermoscopy revealed broken hairs, black dots and pustules and the Wood´s lamp examination was negative. There were no local adenopathies. His past medical history was unremarkable. A recent contact with a cat was described. There was no history of fever or a recent travel.
A hair sample was obtained for mycological examination and he was started on an eight-week course of microsized griseofulvin (15 mg/kg/day orally) and ketoconazole shampoo. Approximately ten days after initiation of therapy, there was a clinical worsening, with transformation into an exudative swelling with purulent discharge, pain and occipital adenopathies (Figure 1). Additional collection of pus for bacteriologic examination was performed. He continued treatment with griseofulvin and was started on topical betamethasone plus gentamicin ointment and clarithromycin (15 mg/kg/day orally), which he completed for seven days. Because of persistent signs of inflammation, despite the negativity of the bacteriological examination, he was switched to amoxicillin plus clavulanic acid (90 mg/kg/day orally), which he continued for another seven days. The inflammation progressively improved, with complete resolution with residual alopecia (Figure 2). Seven weeks after diagnosis, the scalp scraping mycologic examination revealed Trichophyton tonsurans.
Figure 1. Subcutaneous nodule with purulent discharge.
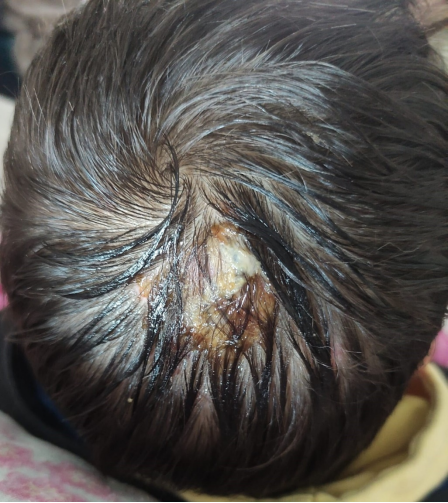 Figure 2.
Figure 2. Progressive resolution of the lesion with residual alopecia.  What is the diagnosis?
|
Discussion :
Anthropophilic and zoophilic dermatophytes are the most common causes of tinea capitis, with Trichophyton spp and Microsporum spp being the most common causes, respectively. 1,2 An increasing number of cases of Trichophyton tonsurans have been observed in Europe. 1,2 Kerion is a rare and severe inflammatory form of tinea capitis resulting from an intense immune response to dermatophytes, characterized by tender, erythematous, purulent swelling with associated alopecia and regional lymphadenopathy. 2,3,4 Trichophyton tonsurans, an anthropophilic endothrix dermatophyte, is most commonly found in asymptomatic carriers and causes non-inflammatory tinea capitis, whereas inflammatory tinea capitis usually results from Microsporum canis infection, although one published study described nearly 30% of cases of kerion in patients infected with Trichophyton tonsurans. 5
To avoid inappropriate treatment and alopecia, the local fungal epidemiology should be known. 1,2,4 Our patient lived in the Lisbon metropolitan area, where Microsporum audouinii and Trichophyton soudanense are the main causes of tinea capitis, with Trichophyton tonsurans being present in almost 10% of the cases described. 6
Based on the epidemiology, history and physical examination we decided to treat with griseofulvin, which is a first-line therapy for tinea capitis. Although terbinafine has been reported to be more effective against Trichophyton tonsurans, the authors decided to keep griseofulvin considering the adequate clinical response to this therapeutic option. 5,7
The use of corticosteroids remains controversial, but some authors recommend it to minimize the risk of scarring alopecia and to minimize the dermatophyte response. 8
Concomitant topical therapies such as shampoos or fungicidal creams or lotions may help to remove scales and spores. 1
Conclusion
Tonsurans infection must be considered in the inflammatory course of tinea.
Kerion can be misdiagnosed as a bacterial abscess, leading to unnecessary antibiotic or surgical intervention. | References : | - Lapergola G, Breda L, Chiesa PL, et al. Kerion celsi caused by Trichophyton tonsurans in a child. Lancet Infect Dis. 2018;18(7):812.
- Tonin B, Geat D, Girolomoni G. A case of kerion celsi caused by Trichophyton tonsurans. Pediatrics International. 2020;62(8):1007-1008.
- Yasuda-Sekiguchi F, Kamata A, Hosokawa R, et al. A Case of Kerion Celsi Caused by Trichophyton Tonsurans, a Plate Culture of Which Showed Yellow-Green Fluorescence Under UVA Light.; 2022.
- Grijsen ML, de Vries HJC. Kerion. CMAJ . 2017;189:E725.
- Dascalu J, Zaaroura H, Renert-Yuval Y, et al. Pediatric Tinea Capitis: A Retrospective Cohort Study from 2010 to 2021. Journal of Fungi. 2023;9(3):366.
- Rato M, Costin A, Furtado C, et al. Epidemiologia das infeções fúngicas superficiais em Portugal - revisão de 3 anos (2014-2016). Journal of the Portuguese Society of Dermatology and Venereology. 2018;76(3):269-278.
- Chen X, Jiang X, Yang M, et al. Systemic antifungal therapy for tinea capitis in children. Cochrane Database of Systematic Reviews. 2016;2016(5).
- Gómez-Moyano E, Fernández-Sánchez AM, Crespo-Erchiga V, et al. Kerion Celsi caused by Trichophyton tonsurans with dermatophytid reaction. Rev Iberoam Micol. 2021;38(3):151-152.
|
|
| Correct Answers : |  100% 100% |
Last Shown : Mar 2026
|