Dr Vishal Dublish1, Dr Ira Shah2.
1Medical Sciences Department, Pediatric Oncall, Mumbai, India,
2Incharge,Pediatric Tuberculosis, HIV and Liver Clinic,B.J.Wadia Hospital for Children, Mumbai.
ADDRESS FOR CORRESPONDENCE
Dr Ira Shah, 1/B Saguna, 271/B St Francis Road, Vile Parle (W), Mumbai 400056. India. | Introduction
Dengue: It is a mosquito borne viral illness. Dengue epidemics have been known since last 300 years. West Indies noticed epidemic in 1635. First confirmed epidemic was reported from Philippines in 1953-1954. Since then Southeast Asia is experiencing major outbreaks with increasing morbidity and mortality. Some countries are having Dengue outbreaks every year.
Problem statement:
Since last 20 years, there is global increase in frequency of Dengue infection.
2.5 - 3.0 billion people are currently at risk worldwide.
Worldwide 50-100 million cases are being reported annually.
Each year approximately 5,00,000 cases of Dengue hemorrhagic fever (DHF) require hospitalization, including 90% children less than 15 years of age. Mortality of Dengue hemorrhagic fever is approximately 5% with 25,000 deaths reported each year.
Usually it is considered an urban disease but now spreading its tentacles in rural areas also.
Indian perspective:
India, Sri Lanka and Myanmar are considered hyperendemic for Dengue fever because of significant increase in the proportions of dengue cases with severe disease. According to WHO, in India, Dengue Hemorrhagic fever is an emergent disease in view of frequent cyclical epidemics and circulation of multiple virus serotypes at present.
Dengue virus:
It is member of Genus flavivirus and family flaviviridae, having single stranded RNA with 4 serotypes: DEN - 1, 2, 3, and 4. All serotypes have potential for causing epidemic and are antigenically similar but different enough to elicit cross protection for only a few months after infection by any of them.
Vector:
Dengue virus is transmitted from person to person by Aedes mosquito. A.aegypti is the most important epidemic vector. Vertical transmission from mother to child has been reported from Bangladesh and Thailand.
Host factor:
Dengue virus infects humans and lower primates. Human (Man) is considered as its urban reservoir. Studies in Africa and Malaysia demonstrated that monkeys are infected with Dengue virus and are the likely reservoir hosts.
Factors associated with resurgence of Dengue epidemics:
- Unprecedented growth of human population
- Unplanned and uncontrolled urbanization
- Inadequate waste management and water supply.
- Increased distribution and densities of vector mosquitoes Lack of effective mosquito control measures
- Increased movement and spread of dengue virus.
Transmission:
Female aedes mosquito gets infected with Dengue virus after sucking blood from a person during viremic (acute febrile illness) phase. After an extrinsic incubation period of 8-10 days, infected mosquito transmits infection by biting and injecting infected salivary fluid into the wound of another person. After an incubation period of 3-14 days (4-6 days average), there is sudden onset of disease with fever, anorexia, malaise, headache, nausea, vomiting and rash etc. Viremia starts just before the onset of symptoms and persists for 5-6 days after the onset of illness. Infected female mosquito is capable of vertical transmission of Dengue virus to its next generation, important for virus maintenance but not for epidemics.
Pathogenesis:
It is not fully understood. It is hypothesized that there is enhancement of virus multiplication in macrophages by heterotypic antibodies which were formed during previous dengue infection.
Two pathophysiologic changes occur predominantly:
- Increased vascular permeability causing selective plasma leakage (pleural, peritoneal) and hypovolemia.
- Abnormal hemostasis resulting from vasculopathy and coagulopathy with thrombocytopenia causing hemorrhagic manifestations.
One study from Vietnam proposed that endothelial size dependent sieving mechanism for plasma proteins is at least primarily retained whereas selective restriction based on negative charge is impaired. Role of anion glycosaminoglycan (GAG) in pathogenesis of vascular leak was suggested. Study from Germany proposed that there may be turbulence of antioxidant system in response and / or consequence of viral inflammatory process. A study from Vietnam suggested that over production of both proinflammatory cytokines (Interferon and Tumor necrosis factor - a) and anti-inflammatory cytokines (IL-10, 6) may play a role in pathogenesis of DHF/DHS.
Pathogenesis of Dengue: table 1
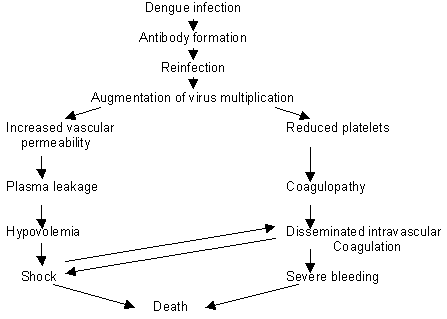
Clinical presentation: Table 2
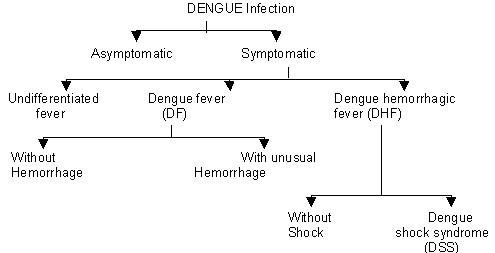
Infection with one Dengue serotype provides lifelong immunity to that particular serotype but there is no overprotection for other serotypes.
Clinical presentation depends upon the age, immune status of the host and virus strain.
Undifferentiated fever:
When there is dengue infection for the first time (primary Dengue infection). It presents like a simple viral fever especially in infants, children or in some adults. Maculopapular rash may or may not be present. Dengue fever: Most commonly seen in older children and adults. Presents as acute biphasic fever with myalgia, arthralgia (Break bone fever), headache, rash, leukopenia and occasionally with unusual hemorrhage.
Dengue hemorrhagic fever:
Children less than 15 years are the most common victims. It presents with acute onset of fever with nonspecific constitutional symptoms and signs of hemorrhagic diathesis, which may progress to fatal shock (Dengue shock syndrome, DSS).
Dengue fever (DF):
Incubation period is 4-6 days (3-14 days range).
Non-specific symptoms such as Headache, backache, malaise, sudden rise of temperature (biphasic) and facial flushing are seen.
Within 24 hours patients have photophobia, retro-orbital pain, pain in back, limbs, joints and bones.
Other clinical features include anorexia, abdominal pain, constipation, altered taste sensations, depression etc.
Rash is diffuse, flushing with pin point eruptions on face, neck, chest which may be maculopapular or scarlentiform. Rash fades away after defervescence of fever.
Skin hemorrhage - either positive tourniquet test and/or petechiae may be present. Some times associated with hemorrhagic complications e.g., epistaxis, gum bleeding, gastrointestinal bleeding, hematuria, hypermenorrhoea etc.
DF with hemorrhagic complications must be differentiated from Dengue hemorrhagic fever (DHF).
Lab findings:
CBC - Normal / leucopenia
Platelet count - Usually normal
PT / PTTK - Normal
Serum biochemistry - Normal
Liver enzymes - Normal / raised.
Differential diagnosis - Various viral/bacterial/parasitic or rickettsial infections
Dengue hemorrhagic fever / Dengue shock syndrome (DHF / DSS):
Typically presents with high fever with hemorrhagic manifestations, liver enlargement with or without circulatory failure and thrombocytopenia.
Abnormal hemostasis with plasma leakage causes rise in hematocrit.
Sudden rise in temperature, pharyngeal congestion, abdominal pain, febrile convulsion are common.
Most common hemorrhagic phenomenon is positive tourniquet test, and early bruising with bleeding at venepuncture sites.
Rash is fine petechial or confluent on face, extremities, axilla, soft palate. Rash may be maculopapular also.
Epistaxis, gum bleeds, gastrointestinal hemorrhages occur occasionally. Rarely hematemesis may be seen.
Study from Chennai, India concluded that a combination of:
Biphasic pattern of fever
Hemoconcentration
Platelet count < 50,000/mm3
Raised aminotransferases.
Prolonged prothrombin time
had a sensitivity of 79.2%, specificity of 64.7%, positive predictive value of 70% and negative predictive value of 75% in predicting spontaneous bleeding in Dengue infection.
Hepatomegaly can be tender in DSS. Jaundice is unusual and splenomegaly in rare in infants.
Chest X-Ray may show pleural effusion (more on right side).
Mild to moderate cases:
Fever subsides with profuse sweating. Mild changes in pulse rate and blood pressure may be noticed with cold extremities and skin congestion. Patient recovers spontaneously or after fluids and electrolyte therapy.
Severe cases:
Sudden deterioration may after few days. Fever subsides in 3-7 days and signs of circulatory collapse appear. Skin becomes cool, congested with circumoral cyanosis, weak and rapid pulse, acute abdominal pain and narrow pulse pressure (< 20 mm Hg). Consciousness is usually intact. Patient may die of profound shock if untreated or recovers after volume replacement. Complications include metabolic acidosis, severe gastrointestinal bleeds, intracranial hemorrhage, convulsions, encephalitis etc. Survivors recover within 2-3 days. Return of appetite is a good prognostic sign. During convalescent stage, bradycardia or arrhythmia may be noted.
Lab investigations:
CBC: Total leukocyte counts may be normal or leukopenia with relative lymphocytosis (> 15% atypical lymphocytes).
Platelet count is reduced
Hematocrit is Increased (> 20%) - suggesting increased vascular permeability and plasma leakage.
Urine - Transient and mild albuminuria.
Stool - Occult blood may be present
PT/PTTK - Prolonged, increased thrombin time.
Decreased fibrinogen, factor VIII, XII, antithrombin-III.
Decreased serum complement.
Severe liver dysfunction with reduced vitamin-K dependent factors and low serum proteins with raised aminotransferases.
Criteria for clinical diagnosis of DHF / DSS :
- Acute onset fever. Continuous and high grade after 2-7 days.
- Hemorrhagic manifestations - (including at least positive tourniquet test), petechiae, purpura, ecchymosis, epistaxis gum bleeds, hematuria, malena etc.
- Hepatomegaly
- Shock - Rapid, weak pulse with narrow pulse pressure (< 20%), hypotension, cold clumsy skin and restlessness.
Laboratory criteria:
- Thrombocytopenia (< 1 lakh/mm3).
- Hematocrit increased by > 20%.
Fever, hemorrhagic manifestations, thrombocytopenia with rising hematocrit are sufficient for clinical diagnosis of dengue hemorrhagic fever (DHF). pleural effusion and hypoalbuminemia are supportive evidences.
Grading of Severity of DHF:
- Fever, non-specific constitutional symptoms. The only positive hemorrhagic manifestation is a positive tourniquet test.
- Above manifestations + spontaneous bleeding in skin and/or other hemorrhages.
- Circulatory failure - rapid and weak pulse, narrow pulse pressure (< 20 m Hg) etc.
Differential diagnosis - Viral, bacterial, protozoal infection. Leptospirosis, malaria, infectious hepatitis, meningococcemia, rubella, influenza.
Complications:
Encephalitis - convulsions, coma, spasticity, paresis etc, because of intracranial bleeds, dic, use of hypotonic fluids to treat DHF patients with hyponatremia (water intoxication). Few evidence suggest that dengue virus infects brain and crosses blood brain barrier. Encephalitis may occur because of acute liver failure and renal failure.
Other rare complications include Acute renal failure, Rhabdomyolysis, splenic rupture, hemolytic uremic syndrome, Gullian Barre syndrome, intravascular hemolysis in cases of hemoglobinopathies or G6PD deficiency. Dual infection with leptospirosis or viral hepatitis-B has also been reported.
Definitive diagnosis :
Confirmatory lab studies for dengue virus infection include:
Isolation of virus - Most definitive but not feasible and requires time, skills, expertise and equipments.
Demonstration of rising titre of specific dengue antibodies.
Demonstration of specific viral antigen/RNA in the tissue or serum.
Serological tests:
Haemagglutination inhibition test: Easy, simple and ideal for seroepidemiological studies. Haemagglutination inhibitor antibodies appear by day 5-6 of illness but this test lacks specificity.
Compliment fixation test: Difficult to perform. Not specific for secondary infections.
Neutralizing test: Most specific and sensitive but technically difficult and time consuming.
IgG ELISA: Can be used to differentiate primary and secondary Dengue infection. But non-specific and cross reacts with other flaviviruses. Does not give serotype diagnosis.
IgM capture ELISA: Widely used, simple and rapidly defects Dengue specific IgM antibodies by capturing them out of solution using antihuman IgM previously bound to the solid phase. After day 5, IgM in detectable and increased in secondary infections. IgM levels reduce in 60 days. Because of persistence of IgM antibodies. MAC ELISA positive results on single serum samples do not necessarily mean that Dengue infection is current but proves that Dengue infection has occurred in last 2-3 months. (AuBio Dot is a multi step visual diagnostic immunoassay, based on IgM capture ELISA, with sensitivity of 97.7% and specificity of 97%).
Rapid serologic test kits: Number of commercial kits are available for detection of anti Dengue IgM or IgG antibodies. But their accuracy is not validated and should not be used in clinical settings to guide management of DF / DHF. These can be used as preliminary screening devices only.
RT-PCR: Useful diagnostic test for confirmation of Dengue virus infection (primary or secondary).
Management:
Early diagnosis and treatment reduces mortality and morbidity.
Dengue fever:
Symptomatic and supportive treatment.
Bed rest during acute febrile illness.
Avoidance of antipyretics / aspirin because of gastritis and bleeding. paracetamol may be given.
Analgesics / mild sedation for pain.
For vomiting and sweating, oral fluids and electrolytes must be supplemented.
Monitoring of patient is required till he becomes afebrile, has normal platelet count and normal hematocrit.
DHF:
Prognosis of DHF depends on early recognition of plasma leakage by frequent estimation of hematocrit (> 20%) and platelet count.
Early volume replacement with isotonic saline reduces severity and prevents shock.
Indications of hospitalization:
Rising hematocrit
Platelet count < 50,000/cumm
Hemorrhagic manifestations.
Fever - No salicylates should be given. paracetamol is safe.
High fever, vomiting and anorexia may cause dehydration. ors or fruit juice may be given.
Close monitoring for shock is mandatory. The critical period between transition from febrile to afebrile phase is approximately 3 days.
Serial hematocrit (or hemoglobin) should be done daily until defervescence.
Volume replacement - Volume should be replaced judiciously and rate of administration should be adjusted by serial hematocrit monitoring. Volume replaced should be minimum but sufficient to maintain effective circulation during plasma leakage. During convalescent phase resorption of extravasated plasma occurs. So if fluids are given continuously even after leakage stops, patient may develop ascitis, pleural effusion, pulmonary edema and respiratory distress.
How much to give: Maintenance fluids (Holiday-sager method) + 5-8% deficit.
Choice of fluid: 1/3 - ½ glucose normal saline. Volume and rate of intravenous fluids should be adjusted according to volume and rate of plasma loss which can be monitored by change in hematocrit, vital parameters and urine output.
Danger signs:
Restlessness, lethargy
Cold extremities, circumoral cyanosis
Reduced urine output
Rapid and weak pulse
Narrow pulse pressure (< 20 m Hg)
Hypotension
Sudden increase in hematocrit
Progressively increasing hematocrit despite administration of intravenous fluids.
DSS: It is a medical emergency. Immediate volume replacement is essential.
Table 3: Volume replacement in Dengue Shock syndrome
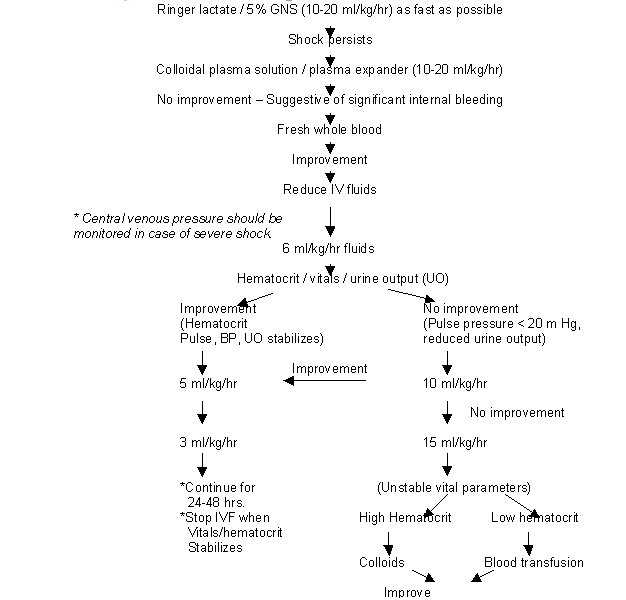
To Discontinue IV fluids:
Hematocrit stabilizes ~ 40%
Improvement in appetite
Urine output - normal
Normal vital parameters.
Dengue fever:
Other supportive measures:
Hyponatremia, metabolic acidosis - judicious use of sodium bicarbonate.
Oxygen - for all shock patients.
Sedation - Chloral hydrate (12.5 - 50 ng/kg) Single dose, Avoid hepatotoxic drugs.
Blood transfusion - Reduced hematocrit without clinical improvement suggests hemorrhage and should be replaced with fresh whole blood. There is no role of preventive transfusion in DSS in sustained improvement in coagulation status.
FFP / Platelet transfusion is required only if severe dic with massive bleeding.
Monitoring should be constant and includes pulse, blood pressure, temperature, hematocrit (2 hourly during 1st 6 hrs and then 4 hourly), input-output chart, IV fluids - type, volume, rate etc.
There is no role of corticosteroids in improving outcome of patients with DHF/DSS.
Prevention and control of dengue fever: At present no specific drug or vaccine is available against dengue virus. So, control primarily is dependent on control of vector.
- Environmental changes: Improving water supply, mosquito proofing of overhead tanks, cisterns and underground reservoirs.
- Personal protection: Protective clothing, mats, coils aerosols (pyrethrum), repellents e.g., Neem oil, DEET, permethrin impregnated in cloth, insecticide treated mosquito nets and curtains. (OLYSET NET).
- Biological control: by
Fish - larvivorous fish: Gambusia affinis and Peorilia reticulata
Bacteria - Bacillus thuringiensis H-14, Bacillus sphaericus - breeds in polluted water.
- Chemical control:
1% temephos sand granules
Space sprays - malathion, fenitrothion, pirimiphos (only in major DHF epidemics).
Insect growth regulators - interfere with development of the immature stages of the mosquito by interference of chitin synthesis during melting process in larvae or disruption of pupal stage.
Dengue Vaccine:
A tetravalent live attenuated DEN vaccine trial has been done in Thailand. After 3rd dose 89% of subjects seroconverted. Trial suggested that this vaccine has moderate but improvable reactogenicity and high seroconversion rates against 4 serotypes of DEN virus after 3rd dose.
A recombinant DEN virus tetravalent vaccine have been developed, which was found to be 92% efficacious in monkeys against all 4 DEN virus serotypes (CHIMERI VAX-DEN).
| | | | Compliance with Ethical Standards | | Funding None | | | | Conflict of Interest None | | |
- Souza LJ, Alves JG, Nogueira RM, Gicovate Neto C et al. Aminotransferase changes and acute hepatitis in patients with dengue fever: analysis of 1,585 cases. Braz J Infect Dis. 2004 Apr;8(2):156-63. Epub 2004 Sep 08. [CrossRef]
- Wills BA, Oragui EE, Dung NM, Loan HT, Chau NV, Farrar JJ, Levin M. Size and charge characteristics of the protein leak in dengue shock syndrome. J Infect Dis. 2004 Aug 15;190(4):810-8. Epub 2004 Jul 19. [CrossRef] [PubMed]
- Davis JS, Bourke P. Rhabdomyolysis associated with dengue virus infection. Clin Infect Dis. 2004 May 15;38(10):e109-11. Epub 2004 Apr 28. [CrossRef] [PubMed]
- De Paula SO, de Melo Lima C, Torres MP, Pereira MR, Lopes da Fonseca BA. One-Step RT-PCR protocols improve the rate of dengue diagnosis compared to Two-Step RT-PCR approaches. J Clin Virol. 2004 Aug;30(4):297-301. [CrossRef]
- Santos NQ, Azoubel AC, Lopes AA, Costa G, Bacellar A. Guillain-Barre syndrome in the course of dengue: case report. Arq Neuropsiquiatr. 2004 Mar;62(1):144-6. Epub 2004 Apr 28. [CrossRef]
- Ahmed S. Vertical transmission of dengue: first case report from Bangladesh. Southeast Asian J Trop Med Public Health. 2003 Dec;34(4):800-3. [PubMed]
- Witayathawornwong P. Parturient and perinatal dengue hemorrhagic fever. Southeast Asian J Trop Med Public Health. 2003 Dec;34(4):797-9. [PubMed]
- Janjindamai W, Pruekprasert P. Perinatal dengue infection: a case report and review of literature. Southeast Asian J Trop Med Public Health. 2003 Dec;34(4):793-6. [PubMed]
- Guirakhoo F, Pugachev K, Zhang Z, Myers G, Levenbook I, Draper K, Lang J et al. Safety and efficacy of chimeric yellow Fever-dengue virus tetravalent vaccine formulations in nonhuman primates. J Virol. 2004 May;78(9):4761-75. [CrossRef] [PMC free article]
- Shepard DS, Suaya JA, Halstead SB, Nathan MB, Gubler DJ, Mahoney RT, Wang DN, Meltzer MI. Cost-effectiveness of a pediatric dengue vaccine. Vaccine. 2004 Mar 12;22(9-10):1275-80. [CrossRef]
- Chakravarti A, Parthasarathy P, Chakravarti A. Evaluation of a rapid immunochromatographic test in the diagnosis of dengue fever. Indian J Pathol Microbiol. 2003 Jan;46(1):127-8. [PubMed]
- Sabchareon A, Lang J, Chanthavanich P, Yoksan S, Forrat R, Attanath P et al. Safety and immunogenicity of a three dose regimen of two tetravalent live-attenuated dengue vaccines in five- to twelve-year-old Thai children. Pediatr Infect Dis J. 2004 Feb;23(2):99-109. [CrossRef]
- Shivbalan S, Anandnathan K, Balasubramanian S, Datta M, Amalraj E. Predictors of spontaneous bleeding in Dengue. Indian J Pediatr. 2004 Jan;71(1):33-6. [CrossRef]
- Donoso Mantke O, Lemmer K, Biel SS, Groen J, Schmitz H, Durand JP, Zeller H, Niedrig M. Quality control assessment for the serological diagnosis of dengue virus infections. J Clin Virol. 2004 Feb;29(2):105-12. [CrossRef]
- Nguyen TH, Lei HY, Nguyen TL, Lin YS, Huang KJ et al. Dengue hemorrhagic fever in infants: a study of clinical and cytokine profiles. Infect Dis. 2004 Jan 15;189(2):221-32. Epub 2004 Jan 09. [CrossRef]
- Miranda LE, Miranda SJ, Rolland M. Case report: spontaneous rupture of the spleen due to dengue fever. Braz J Infect Dis. 2003 Dec;7(6):423-5. Epub 2004 Mar 01. [CrossRef]
- Lum LC, Abdel-Latif Mel-A, Goh AY, Chan PW, Lam SK. Preventive transfusion in Dengue shock syndrome-is it necessary? J Pediatr. 2003 Nov;143(5):682-4. [CrossRef]
- Vazquez S, Lemos G, Pupo M, Ganzon O, Palenzuela D, Indart A, Guzman MG. Diagnosis of dengue virus infection by the visual and simple AuBioDOT immunoglobulin M capture system. Clin Diagn Lab Immunol. 2003 Nov;10(6):1074-7. [PMC free article]
|
| Cite this article as: | | Shah I, Dublish V. DENGUE AND DENGUE HEMORRHAGIC FEVER DENGUE SHOCK SYNDROME. Pediatr Oncall J. 2005;2: 48. |
|