Introduction
Retinopathy of Prematurity (ROP) is a retinal vascular disease affecting premature newborns of low birth weight. The smaller and younger the neonate, the greater is the risk for this potentially blinding disease. Apart from prematurity and low birth weight, excessive oxygen use, and various neonatal illnesses are risk factors.
Twenty-two percent of the burden of childhood blindness can be attributed to retinal disease, of which ROP is an important cause1. At least 50,000 children worldwide are estimated to be blind due to retinopathy of prematurity and the number is ever-increasing2.
While progress in neonatology has seen an increase in survival rates of extremely low birth weight babies (ELBW)3, there has been a corresponding rise in the incidence of Retinopathy of prematurity4.
Indian studies have shown that in low birth weight babies, the incidence of ROP varies from 38-51.9%5,6,7.
India is now considered at high risk for retinopathy of prematurity, as it is a country whose neonatal care services have improved with better survival rates, while at the same time the existing screening protocols and level of care for ROP are not adequate. Thus has emerged what is considered to be the ‘Third Epidemic of ROP’ of which India, along with several middle-income nations, is a part.8
The pediatrician and the neonatologist are the first line of defense against this epidemic. While the preterm newborn is at risk of the disease, it must be emphasized that the baby does not have the disease at birth. ROP develops typically by 3-4 weeks of life, yielding a golden window period for detection and treatment. Thus the timely referral of the ‘at risk’ babies to the ophthalmologist for screening is crucial in the final visual outcome.
Recognizing the urgency, the Ministry of Health and Welfare, India has included Retinopathy of prematurity in the screening guidelines of newborns in the ‘Rashtriya Bal Swasthya Karyakram’ (an initiative launched in 2013)9. ‘The India Newborn Action Plan’ launched in September 2014 by the Health Minister of India, once more emphasizes ROP screening in the ‘Care of the small and sick newborn’ section of the plan10.
Retinopathy of Prematurity - History
ROP is a fairly new disease and was first described by Terry in the 1940s11.
1942: Terry identified the disease & coined the term ‘Retrolental Fibroplasia’.11
1951: Campbell suggested that the toxic effects of oxygen in the neonates caused the disease12.
1952: Heath coined the term Retinopathy of Prematurity, which became the more accepted nomenclature12.
1953: Studies proved that high concentrations of oxygen were causative12.
Retinopathy of Prematurity - Etiopathogenesis
Development of retinal vasculature13
The retina is avascular to 14 weeks of intrauterine life. At around the 4th month of gestation, the vascular complexes grow from the optic disc outwards towards the periphery, in the form of an expanding vascular apron. The vasculature reaches the nasal ora Serrata at 8 months of gestation; however, the temporal retina is not completely vascularised until 1 month after delivery
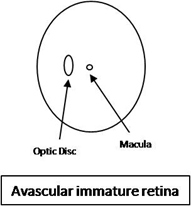
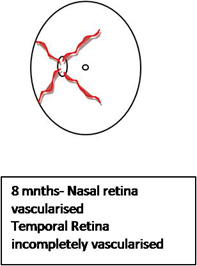
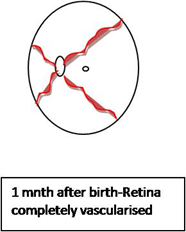
Theories of Pathogenesis
- Classical Theory (Ashton Patz)14: Oxygen is implicated as the major causative factor. Hyperoxia occurs due to high concentrations of oxygen given to the baby. This causes a retinal arteriolar spasm which later on becomes permanent closure. When the neonate returns to room air, there is endothelial proliferation adjacent to the closed vessels leading to neovascularization and retinal traction.
- Spindle cell or Gap Junction theory (Kretzer)15: The avascular retina of the premature neonate contains spindle cells. These cells are attacked by the toxic oxygen metabolites limiting their migration and canalization. Gap junctions are formed between adjacent spindle cells, through which abnormal vessels erupt.
- Current Theory or Growth Factor theory16: Vascular Endothelial Growth Factor (VEGF) plays an important role in the vascularisation of the normal retina. In conditions of increased oxygen saturation, VEGF is inhibited, thus resulting in the avascular retina. This hypoxic retina shows a rebound increase in VEGF leading to uncontrolled neovascularization.
Risk Factors
The risk factors for ROP are listed below17,18:
- Prematurity and low birth weight
- High oxygen levels
- Septicemia
- Acidosis
- Hyperglycemia
- Multiple gestation
- Anemia
- Respiratory distress syndrome
- Apnoeic spells
- Intraventricular hemorrhage
Retinopathy of Prematurity - Symptoms
Ideally, the disease is picked up at an asymptomatic stage by a screening of at-risk neonates.
However it is common that the parents directly present at a later stage with the complaints of: -
- Inability of the child to see
- Abnormal pendular or searching movements of the eyes
- White reflex in the pupillary area (when the child has the stage 5 disease which Terry had described as Retrolenticular Fibroplasia).
In modern times, with the various studies done and treatment options available, a neonate at risk developing advanced disease without having had an ophthalmic check-up or referral done, can have severe medicolegal repercussions for the primary treating pediatrician or neonatologist.
Retinopathy of Prematurity - Examination
The pupillary reaction is assessed with the help of torchlight or the indirect ophthalmoscope with the aid of the 20 Dioptre lens for magnification. A rigid pupil that does not even respond to dilating drops is a sign of ‘Plus Disease’ (described later) indicating a tendency to progression. The neonate at risk is examined by Indirect Ophthalmoscopy. The pupil is dilated with tropicamide 0.5-1% with phenylephrine 2.5%19. Cyclopentolate 0.5-1% can also be used19. A single drop is instilled in each eye 5-10 minutes apart and 2-3 installations are usually adequate19.
Atropine drops or ointment are not to be used for dilation as tachycardia, hyperthermia or severe dehydration can occur in premature babies. In India, Phenylephrine drops are available in 10% concentration and can be diluted (1:4) with distilled water or a lubricant to get a concentration of 2.5%19.
Diagnosis And Categorization
The diagnosis of ROP is made by an indirect ophthalmoscopic examination. The complete diagnosis also should have a description of the magnitude of the disease.
An International Classification of Retinopathy of Prematurity (ICROP) was presented in 1984 (and then revised in 2005), which describes the magnitude, in the form of ‘Zones’, ‘Extent’ and ‘Stages’ of the disease and whether ‘Plus disease’ is present or absent.20. These descriptions help to define which neonates can be observed and which require treatment.
Zones
| Zone 1 |
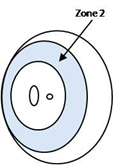
Zone 2 |
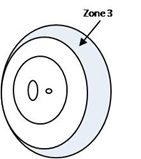
Zone 3 |
| Lies within a circle centred on the disc of radius equal double the distance between the disc and the foveola. |
Lies outside zone1, bound externally by a circle concentric to that of zone 1, the radius of which is the distance from the disc to the nasal ora serrata |
It is the temporal crescent of retina which lies outside zone 2. |
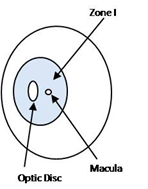
Extent
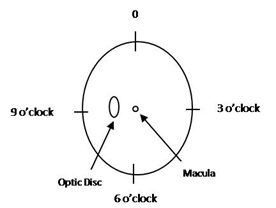
The extent is described in terms of the number of clock hours involved20.
Stages20
The more premature the baby, the less of the retina is vascularized. The avascular hypoxic retina is opaque, while the well-vascularised retina is transparent and the junction between the two has a demarcation line. Branching vessels within the plane of the retina are often seen running till the demarcation line (Stage 1).
If it progresses the line acquires height and volume and now appears like a pink or white ridge (Stage 2).
Continued VEGF production causes extraretinal fibrovascular proliferation, which is recognized by vessels growing from the ridge into the vitreous (Stage3). The Fibrous tissue then begins to contract, exerting a pull on the retina (Stage 4). In advanced disease, the entire retina is detached (Stage 5).
| Stage |
Description |
| Stage 0 |
Immature vascularisation, no ROP |
| Stage 1 |
Demarcation Line |
|
Stage 2
|
Ridge ± tufts of fibrovascular proliferation
|
|
Stage 3
|
Extraretinalfibrovascular proliferation
|
|
Stage 4
|
Subtotal Retinal Detachment
- Extrafoveal
- Involving the fovea
|
|
Stage 5
|
Total Retinal Detachment
|
Plus Disease and Preplus Disease
Plus disease was described by the International Classification of Retinopathy of Prematurity (ICROP) in 1984, as ROP in which there was engorgement of retinal veins and tortuosity of arterioles20. It occurs due to vascular shunting through the neovascularisation and indicates severe disease. Other features include vitreous haze, dilated iris vessels, nondilating pupil.
In the 2005 modification of the ICROP the definition of Pre plus disease was added, which described dilated tortuous veins, but to a lesser degree than that seen in plus disease20.
Threshold disease & Prethreshold disease
The definitions of threshold and pre threshold disease are important for decision making regarding treatment.
The multicenter trial for cryotherapy for retinopathy of prematurity (CRYO ROP), defined threshold disease as ‘5 contiguous or 8 cumulative clock hours of stage 3 disease in Zone I or II, with Plus disease’21. Neonates with threshold disease should be treated, as they have a 50% chance of progression to retinal detachment if left untreated.
The Early Treatment of Retinopathy of Prematurity trial (ETROP) explored the need for treatment even before threshold disease and defined Prethreshold disease which is further classified into types 1 & 222.
| Type 1 |
Zone I any stage with plus disease
Zone I any stage 3 without plus disease
Zone II stage 2 or 3 with plus disease
|
| Type 2 |
ZoneI stage 1 or 2 without plus disease
Zone II stage 3 without plus disease
|
Aggressive Posterior ROP (APROP)
Along with pre plus disease, the 2005 modification of the ICROP also described APROP also called ‘Rush Disease’. The disease involves the posterior pole and progresses rapidly without necessarily going through the classic stages20. This disease affects the lowest birth weight babies. The fundus shows ‘brush-like neovascularisation’ with shunting of blood from arterioles to venules such that both become tortuous and dilated and it becomes difficult to differentiate between the two. Since there is rapid progression to stage 5 disease, urgent treatment is warranted20.
Retinopathy of Prematurity - Natural History
80% of the time, ROP regresses spontaneously, with the fibrovascular structures becoming fibrotic. The more florid the disease at the time of involution, the more severe are the cicatricial sequelae13. The stages of cicatrization are given as follows:-
Stage 1: Shows peripheral retinal disturbances
Stage 2: There is straightening out of the temporal retinal vascular arcades, with peripheral vitreoretinal fibrosis. There is ‘dragging’ of the macula temporally due to the fibrosis.
Stage 3: Excessive fibrosis results in a falciform retinal fold.
Stage 4: Partial retinal detachment.
Stage 5: Complete ring of retro lenticular fibrovascular tissue with total retinal detachment.
1. Patel DK, Tajunisah I, Gilbert C, Subrayan V. Childhood blindness and severe visual impairment in Malaysia: a nationwide study. Eye (Lond). 2011 Apr;25(4):436-42.
2. Gilbert C. Retinopathy of prematurity: a global perspective of the epidemics, population of babies at risk and implications for control. Early Hum Dev. 2008 Feb;84(2):77-82.
3. Hack M, Fanaroff AA. Outcomes of children of extremely low birthweight and gestational age in the 1990s. SeminNeonatol. 2000 May;5(2):89-106.
4. Valentine PH, Jackson JC, Kalina RE, Woodrum DE. Increased survival of low birth weight infants: impact on the incidence of retinopathy of prematurity. Pediatrics. 1989 Sep;84(3):442-5.
5. Gopal L, Sharma T, Ramchandran S, Shanmugasundaram R, Asha V. Retinopathy of prematurity. A study. Indian J Ophthalmol 1995;43:50-61
6. Charan R, Dogra MR, Gupta A, Narang A. The incidence of retinopathy of prematurity in a neonatal care unit. Indian J Ophthalmol 1995;43:123-26.
7. Varughese S, Jain S, Gupta N, Singh S, Tyagi V, Puliyel JM. Magnitude of the problem of retinopathy of permaturity. Experience in a large maternity unit with a medium size level-3 nursery. Indian J Ophthalmol 2001:49:187-88.
8. Gilbert C. Changing challenges in the control of blindness in children. Eye (Lond). 2007 Oct;21(10):1338-43.
9. Rashtriya Bal Swasthya Karyakram, Operation guidelines. Ministry of Health and Family Welfare, India Government.http://nrhm.gov.in/images/pdf/programmes/RBSK/Operational_Guidelines/Operational%20Guidelines_RBSK.pdf
10. The India Newborn Action Plan. Ministry of Health and Family Welfare, India Government, 2014. http://www.newbornwhocc.org/INAP_Final.pdf
11. Chakrabarti M, Stephen V,Rani S, Chakrabarti A. Retinopathy of Prematurity: Screening and Management. Kerala Journal of Ophthalmology. 2007 Dec: 429-38.
12. RETROLENTAL fibroplasia. Br Med J. 1953 Sep 12;2(4836):610-1.
13. Kanski J, Bowling B. Clinical Ophthalmology: A systematic approach. 6th Ed. China: Elsevier; 2011.
14. A. Patz, L.E. Hoeck, E. DeLaCruz, Studies on the effect of high oxygen administration in retrolental fibroplasia: I. Nursery observations, Am. J. Ophthalmol. 35 (1952) 1248–1252.
15. Kretzer FL, Hittner HM. Human retinal development: relationship to the pathogenesis of retinopathy of prematurity. In: McPherson AR, Hittner HM, Kretzer FL, eds. Retinopathy of prematurity: current concepts and controversies. Toronto: Decker, 1986: 27-52.
16. Smith LE. Pathogenesis of retinopathy of prematurity. Growth Horm IGF Res. 2004 Jun;14Suppl A:S140-4.
17. Kim, T.-i., Sohn, J., Pi, S.-y. and Yoon, Y. H. (2004), Postnatal risk factors of retinopathy of prematurity. Paediatric and Perinatal Epidemiology, 18: 130–134.
18. Holmstrom G, Broberger U, Thomassen P. Neonatal risk factors for retinopathy of prematurity –a population-based study. ActaOphthalmologicaScandinavica. 2003:204-07.
19. Jalali S, Anand R, Kumar H, Dogra MR, Azad R, Gopal L. Programme planning and screening strategy in retinopathy of prematurity. Indian J Ophthalmol 2003;51:89-97.
20. International Committee for the Classification of Retinopathy of Prematurity. The International Classification of Retinopathy of Prematurity revisited. Arch Ophthalmol. 2005 Jul;123(7):991-9.
21. Multicenter trial of cryotherapy for retinopathy of prematurity. Preliminary results. Cryotherapy for Retinopathy of Prematurity Cooperative Group. Arch Ophthalmol. 1988 Apr;106(4):471-9.
22. Good WV; Early Treatment for Retinopathy of Prematurity Cooperative Group. Final results of the Early Treatment for Retinopathy of Prematurity (ETROP) randomized trial. Trans Am Ophthalmol Soc. 2004;102:233-48; discussion 248-50.
23. Retinopathy of Prematurity. In: Basic and clinical science course (BCSC) Section 6: Pediatric Ophthalmology and Strabismus. San Francisco, CA: American Academy of Ophthalmology; 2012:280-7.
24. Pejaver RK, Vinekar A, Bilagi A. National Neonatology Foundation's Evidence Based Clinical Practice Guidelines for Retinopathy of Prematurity, NNF India, Guidelines, 2010. p. 253-62.
25. Fijalkowski N, Zheng LL, Henderson MT, Wallenstein MB, Leng T, Moshfeghi DM. Stanford University Network for Diagnosis of Retinopathy of Prematurity (SUNDROP): four-years of screening with telemedicine. Curr Eye Res. 2013 Feb;38(2):283-91.
26. Vinekar A, Gilbert C, Dogra M, Kurian M, Shainesh G, Shetty B, Bauer N. The KIDROP model of combining strategies for providing retinopathy of prematurity screening in underserved areas in India using wide-field imaging, tele-medicine, non-physician graders and smart phone reporting. Indian J Ophthalmol. 2014 Jan;62(1):41-9.
27. Jalali S, Azad R, Trehan HS, Dogra MR, Gopal L, Narendran V. Technical aspects of laser treatment for acute retinopathy of prematurity under topical anesthesia. Indian J Ophthalmol. 2010 Nov-Dec;58(6):509-15.
28. Ng EY, Connolly BP, McNamara JA et al. A comparison of laser photocoagulation with cryotherapy for threshold retinopathy of prematurity at 10 years: part 1. Visual function and structural outcome. Ophthalmology 2002;109(5):928-934.
29. Connolly BP, Ng EY, McNamara JA et al. A comparison of laser photocoagulation with cryotherapy for threshold retinopathy of prematurity at 10 years: part 2. Refractive outcome. Ophthalmology 2002;109(5):936-941.
30. Palmer EA, Hardy RJ, Dobson V, Phelps DL, Quinn GE, Summers CG, Krom CP, Tung B; Cryotherapy for Retinopathy of Prematurity Cooperative Group. 15-year outcomes following threshold retinopathy of prematurity: final results from the multicenter trial of cryotherapy for retinopathy of prematurity. Arch Ophthalmol. 2005 Mar;123(3):311-8.
31. Roohipoor R, Karkhaneh R, Riazi-Esfahani M, Ghasemi F, Nili-Ahmadabadi M. Surgical management in advanced stages of retinopathy of prematurity; our experience. J Ophthalmic Vis Res. 2009 Jul;4(3):185-90. PubMed PMID: 23198072; PubMed Central PMCID: PMC3498568.
32. Hartnett ME, Maguluri S, Thompson HW, McColm JR. Comparison of retinal outcomes after scleral buckle or lens-sparing vitrectomy for stage 4 retinopathy of prematurity. Retina.2004;24(5):753–7.
33. Hubbard GB 3rd. Surgical management of retinopathy of prematurity. CurrOpinOphthalmol. 2008 Sep;19(5):384-90.
34. Lakhanpal RR, Fortun JA, Chan-Kai B, Holz ER. Lensectomy and vitrectomy with and without intravitreal triamcinolone acetonide for vascularly active stage 5 retinal detachments in retinopathy of prematurity. Retina. 2006;26(7):736–40.
35. Tsukahara Y, Honda S, Imai H, et al. Autologous plasmin-assisted vitrectomy for stage 5 retinopathy of prematurity: a preliminary trial. Am J Ophthalmol. 2007;144(1):139–41.
36. Law JC, Recchia FM, Morrison DG, Donahue SP, Estes RL. Intravitrealbevacizumab as adjunctive treatment for retinopathy of prematurity. J AAPOS. 2010 Feb;14(1):6-10.
37. Geloneck MM, Chuang AZ, Clark WL, Hunt MG, Norman AA, Packwood EA, Tawansy KA, Mintz-Hittner HA; for the BEAT-ROP Cooperative Group. Refractive Outcomes Following BevacizumabMonotherapy Compared With Conventional Laser Treatment: A Randomized Clinical Trial.JAMAOphthalmol. 2014 Aug 7.
38. Quinn GE, Dobson V, Davitt BV, Hardy RJ, Tung B, Pedroza C, Good WV; Early Treatment for Retinopathy of Prematurity Cooperative Group. Progression of myopia and high myopia in the early treatment for retinopathy of prematurity study: findings to 3 years of age.
39. Kushner BJ. Strabismus and amblyopia associated with regressed retinopathy of prematurity.ArchOphthalmol. 1982 Feb;100(2):256-61.
40. Askie LM, Henderson-Smart DJ, Ko H. Restricted versus liberal oxygen exposure for preventing morbidity and mortality in preterm or low birth weight infants. Cochrane Database Syst Rev. 2009 Jan 21;(1):CD001077.
41. Askie LM. Optimal oxygen saturations in preterm infants: a moving target. Curr Opin Pediatr. 2013 Apr;25(2):188-92.
42. Jalali S. Lecture ROP Dos & Dont's. LV Prasad Eye Institute.http://www.lvpei.org/rop/videos/video3.html
43. Jalali S, Anand R, Rani PK, Balakrishnan D. Impact of the day-30 screening strategy on the disease presentation and outcome of retinopathy of prematurity. The Indian twin cities retinopathy of prematurity report number 3. Indian J Ophthalmol. 2014 May;62(5):610-4.