
Abstract
Context:
Tetanus has its existence from time immemorial but still remains as an unsolved puzzle in terms of its pathogenesis and management. To have better insights into this complex infectious disease, the current mini-review illustrates a brief description of tetanus and its history, latest statistics, and its types followed by pathogenesis which includes causes, and mechanisms of infection. Further, the article highlights on prognosis, duration of incubation, etiology, and diagnosis. The review also amalgamates the possible treatments and preventive measures, complications, with special reference to myths surrounding the disease. Ayurvedic approaches and remedies have also been incorporated for paving newer insights on explorative research to facilitate the search for novel drug targets composed of almost no or lesser side effects, thus promoting human health and societal welfare.
Evidence acquisition:
A detailed review of the literature was performed using search engines and databases (Google Scholar and PubMed Central) using keywords as tetanus AND prevalence, tetanus AND mechanism as reference. The article lists available to date were scrutinized. The extracted manuscripts were analyzed for disease prevalence globally and were thoroughly compiled as a part of data mining. For ayurvedic references, an in-depth search was performed in Charaka, Susrutha, and Nagarjuna literature.
Result:
Increased statistics and with partially understood mechanism, awareness about tetanus is still a lacuna. Further understanding of the disease by research communities will help in eradicating tetanus and also equipped clinicians with a better management approach against this deadly infection which is simply much more complex to be understood.
Keywords:
Clostridium tetani, Tetnospasmin, Tetanolysin, Immunization, Dhanustmbha, and Nirgundi.
Introduction
Tetanus is a non-communicable disease and can be life-threatening without proper treatment. The word tetanus is derived from the Greek word ‘teinein’ meaning ‘to stretch’.1 It is a serious disease caused by bacteria that affects the nervous system and causes the tightening of the whole muscle in the infected host. Synonymically, it is also referred to as lockjaw because it tightens the muscle of the neck and jaws, but can spread to other parts of the body as the disease progresses. Due to the ubiquitous nature of the pathogen, the infection is found globally. According to the Centers for disease control and prevention (CDC), approximately 10 to 20 percent of infections are fatal. Tetanus is a type of infection disorder that demands immediate attention and treatment. Vaccines are available which can prevent the disease but this doesn’t last for long. To maintain immunity against this disease periodic vaccination has to be administered at least once every 10 years.
The history of tetanus dates back to ancient civilization where people knew tetanus very well as they could recognize and correlate between wounds and fatal muscle spasm (undocumented folklore). In 1884, Arthur Nicolaier was the first to isolate tetanus toxin (strychnine) from free-living, anaerobic soil bacteria. Antonio Carle and Giorgio Rattone from the University of Turin were successful in elucidated the etiology of the disease and also demonstrated the transmissibility of tetanus. Tetanus was successfully emulated by them in rabbits by subjected pus cells from an infected patient to their sciatic nerves.2 Kitasato Shibasaburo first isolated Clostridium tetani from humans in 1891 later demonstrated how the bacteria produced disease when subjected to animals and also demonstrated the neutralization of toxin by specific antibodies. Edmond Nocard in 1897 demonstrated the induction of passive immunity by tetanus antitoxin in humans and could be used for prophylaxis and management. The first vaccine for tetanus was established by Descombey in 1924 which was then used for the prevention of tetanus caused by battle wounds during World War II.2
Statistics & demographics
International statistics
Clostridum tetani finds its niche worldwide as a soil habitat and is predominant in underdeveloped countries. Factors that aid its development are warm climate especially summer, cultivated soil, rural areas, and the infection is much more prevalent among males. Lack of proper immunization programs leads to tetanus development especially in neonates and young kids. Developed countries show less occurrence of tetanus. For example, during 1984-1992 in England and Wales only 126 cases were reported. In 1992 with the data yield high neonatal tetanus was observed, which was approximately 578,000 infant death followed by 215,000 deaths in 1998, more than 50% of them were African. Tetanus is one of the targeted diseases for the immunization program by the World Health Organization (WHO). Overall, the annual incidence is 0.5-1 million cases. In 2002 as estimated by WHO, there were 213,000 tetanus deaths, 198,000 among them were kids younger than 5 years.
National statistics
The annual mortality rate in 2017 is 2.4 per 100,000 persons. This has decreased by 86.3% since 1990, at an average of 3.8% a year. Among men, the deadliness of tetanus in India peaks at an age above 80. At age 15-19 the rate is least among men. In 2013, 58 deaths per 100,000 men were reported; the peak mortality rate for men was higher than that of women, which were 13 per 100,000 women. Among women, the death rate is high at an age of 75-79 and least at the age of 50-54.
Age-related demographics
The occurrence of neonatal tetanus is rare and could be found mainly in countries which lack immunization program. Its occurrence is highest in elderly people. As per stats in the U.S. out of 59% cases, 75% of deaths occur in a person aged above 60 years or older. From 1980, 70% of cases were 40 or older, 36% are older than 59 years and 9% were below 20 years of age. This data shows the vulnerability against tetanus with age.
Sex-related demographics
Tetanus affects both sexes. High prevalence is reported in males due to frequent exposure to soil. As per statistics during the year 1998 to 2000 in the U.S, the tetanus incidence was 2.8 times higher in males aged 59 years or younger as compared to females. Here the level of immunity differs between the sexes, in total men are more protected than women because of vaccine administration. In developing countries, women are better protected than men due to immunization of pregnant women to prevent neonatal tetanus. The above data depicts the role of immunization in protection against tetanus infection.
Ethnicity-related demographics
Tetanus is found in all types of races. As per data in the U.S. from 1998 to 2000 High occurrence of Tetanus was observed among Hispanics, followed by Native Americans, and then by African Americans.
Pathogenesis
A major culprit for the disease is a bacterium called Clostridium tetani. Spores of bacteria are found in dust, soil, and animal droppings which facilitate them to spread freely. This robust character makes them a tuff candidate to be eradicated. Moreover, the bacteria are able to tolerate harsh conditions also abiotic/biotic factors are responsible for promoting the infection. Tetanus wounds are often associated with burns, cut wounds, punctured wounds, and are contaminated with soil or saliva. People of all ages can get tetanus but the most vulnerable are the pregnant mother and the newborn child. Neonatal tetanus is prevalent in rural areas due to a lack of proper medical facilities and sterile conditions. The infection occurs worldwide but is prevalent in hot and humid weather.
Neurotoxins are produced by the bacteria in anaerobic conditions mainly in the secondary wound. The spores enter the bloodstream through cut wounds and subsequently spread to the neural system which produces tetanospasmin (neurotoxin). This tetanospasmin blocks the signaling towards motor neurons which affects the muscles. Tetanus also occurs during pregnancy or within 6 weeks after the child is born and is called maternal tetanus while tetanus caused within 28 days of life is called neonatal tetanus.
Pathophysiology
Clostridium tetani is a type of obligate motile anaerobe11 and gram-positive bacillus. It forms non-encapsulated spores that are resilient to heat, dehydration, and sterilization. Colorless spores are located at one end of the poles which resemble a turkey leg. Present in soil, house dust, animal intestines, and human feces. Spores can persist in normal human tissue for months to years. In order to propagate, the spores require specific anaerobic environments, like wounds with low oxidation-reduction potential (for eg: dead or devitalized tissue, foreign body, active infection). These surroundings upon germination, aid to release toxins. Proper anaerobic condition leads to the release of two types of toxins: (a). Tetanolysin - This is a hemolysin with no known pathologic activity. (b). Tetanospasmin - It is a primary toxin that is responsible for the clinical indicators of tetanus; by its molecular weight, it is one of the most potent toxins known, with a least lethal dose of 2.5 ng/kg body weight.
Mechanism of tetanus infection
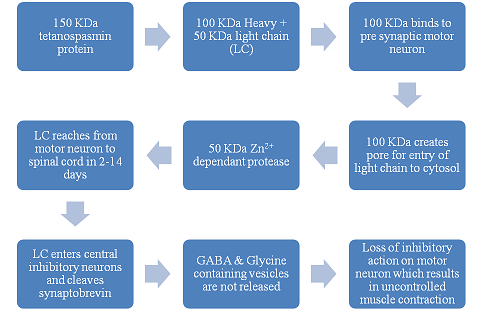
Tetanospasmin is a 150 kD protein (Fig. 2) constitutes of two units of proteins 100 kD heavy chain and 50 kD light chain both linked by a disulfide bond.12 Among them, the heavy chain has two functions one binding of tetanospasmin to presynaptic motor neuron the other is creating pore which facilitates the access of light chain in the cytosol. The light chain is a kind of Zn2+ dependant protease13 which cleaves synaptobrevin. On the entry of the light chain into the motor neuron, it movements by retrograde axonal transport from the location of infection to the spinal cord in 2-14 days. In the spinal cord, it enters the central inhibitory neurons. The light chain cuts the synaptobrevin protein, which is essential for binding the neurotransmitter comprising vesicles to the cell membrane resulting in non-release of GABA (gamma-aminobutyric acid) and glycine from vesicles.13 Further, this leads to loss of central inhibition, creating automatic hyper action resulting in uncontrolled muscle contraction in response to normal stimuli. The passage of the toxin is through the central nervous system which uses motor neurons as a transport cell.14 Fixed toxins on to neurons cannot be neutralized by antitoxin. Recovery requires new nerve terminals and new synapses formation.
Figure 2: Mechanism of action - the forward arrows indicates the molecular mechanism of disease progression.
Presentation
Generalized tetanus
This is a predominant type representing about 80% of cases and is the most widely spread. The generalized form usually shows a downward pattern. The major sign is trismus or lockjaw and the facial tremors called risus sardonicus, followed by neck stiffness, trouble in swallowing, and rigidity of pectoral and calf muscles. Other symptoms are high temperature, perspiring, high blood pressure, and episodic rapid heart rate. Spasms occur in a characteristic form known as opisthotonos (a state of severe hyperextension and spasticity in which an individual’s neck and spinal column enter into a complete bridging position). These symptoms may occur regularly and last for several minutes depending upon the body shape. Seizures last for up to four weeks and comprehensive healing may take months.
Figure 1: Types of tetanus based on their host and clinical symptoms.
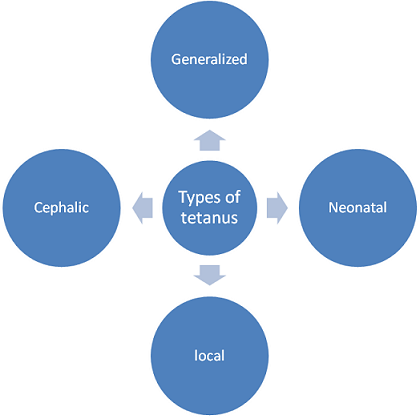
Neonatal tetanus
It’s a type of tetanus that occurs in newborns, this happens to the kids born to unvaccinated mothers. Under maternal vaccination care, the offspring is protected via passive immunity. Many times, due no socio-economical status and/or pre/post-operative surgical devices are known to be the major culprits of infection (especially, the umbilical stump cut with a nonsterile instrument). As per the statistics in 1998, about 14% (215,000) were suffering from neonatal tetanus were reported in developing countries. Due to the public health campaign, the death toll got decreased during the years 1990 and 2010 by 90%. The disease was eliminated in 25 countries and was rare in developed countries by 2013.3 However, the disease still persists in underdeveloped nations that lack the basic facility of mass vaccination.
Local tetanus
This is uncommon in nature and occurs due to persistent contraction of a muscle in a particular muscle area as a result of the injury. The contraction prolongs for many weeks and gradually subsides. This is considered as the milder form of tetanus and reported cases are about 1%.
Cephalic tetanus
This is the rarest form of the disease (0.9-3% of cases)4 and is limited to muscles and nerves present in the head. The main cause is trauma to the head area5, which includes skull breakage, cut6, eye wound5, dental removal7, and otitis media8, nevertheless, it is also linked with injuries to other parts of the body9. Frequent implication is done for paralysis of the facial nerve7,10 which leads to lockjaw, facial palsy, or ptosis, this may affect other cranial nerves as well. Cephalic tetanus may lead to a more generalized form.4,10 Rarity of disease brings unfamiliarity among clinicians5 and might not even suspicious tetanus as a disease. Symptoms may be complex6 and may relate to initial injuries. It is fatal than other types of tetanus with a progression of 15-30% cases4,6,10 to generalized tetanus.
Clinical Features and Diagnosis
The diagnosis is related to the incubation period, it starts from the spore inoculation to the initial symptom and further leading to the first titanic spasm. The following can be concluded (a). Shorter intermissions directly relate to severe tetanus and a poorer diagnosis. (b). Patients usually survive tetanus and get back to their original state of health. (c). Slow recovery usually over 2-4 months. (d). Clinical tetanus does not produce immunity; active immunization is needed to prevent reoccurrence. A high risk of mortality is related to the following: short incubation time, early onset of convulsions, delay in action, and contaminated lesions of the head and the face.
A rating scale has been established to assess the severity of tetanus and shaping the diagnosis.15 On this scale, 1 point is given for each of the following: Incubation period <7 days, Period of onset <48 hours, tetanus which is attained from injuries like burns, surgical wounds, compound fractures, septic abortion, umbilical stump, or intramuscular injection, narcotic addiction, generalized tetanus, temperature >104°F (40°C), tachycardia >120 beats/min (150 beats/min in neonates). The disease diversity and the severity is mentioned in the rating scale mentioned in table no.1.
Table - 1: Rating scale for severity of disease
| Scale |
0-1 |
2-3 |
3-4 |
5-6 |
| Type of tetanus |
Mild |
Moderate |
Severe |
Very Severe |
| Motality% |
<10% |
10-20% |
20-40% |
>50% |
Incubation period
The incubation period may range up to several months but commonly about ten days.16,17 The incubation period also depends upon the distance of the damage to the central nervous system; greater distance is related to longer incubation time. Shorter incubation has extra severity of symptoms.18 In the case of neonatal tetanus, the signs appear from 4 to 14 days after birth and the average is about 7 days. Based on clinical outcomes, four diverse forms of tetanus have been defined2 as discussed above (Fig 1).
Etiology
Tetanus spores are resistant to harsh environments, disinfectants, and also for boiling temperatures up to 20 min which makes their survival easier for some years. Though vegetative cells can be deactivated and are susceptible to numerous antibiotics. Tetanus can be developed in both outdoor and indoor environments. The major basis of infection is wound (approx 65%), often is slight (wood, metal, or thorns) generally no initial medical attention is sought. A prolonged skin ulcer is a source in the case of approx 5% of the cases. In other cases, the obvious source cannot be documented. Tetanus also advances as a problem for chronic conditions like blisters and gangrene. Tetanus possibly infects tissue damage by burns, frostbite, middle ear infection, dental or surgical procedures, abortion, childbirth, and intravenous (IV) or subcutaneous drug use. An important cause of tetanus is lack of immunization it disturbs non-immunized, partly immunized, or full vaccinated persons due to lack of maintenance of periodic booster doses. Universal perils for neonatal tetanus comprise the following: unvaccinated mother, home delivery and unhygienic condition for delivery, past history of tetanus in the previous child is a risk for the successive child, infectious substance attached to the umbilical cord, and vulnerability to tetanus increases with age.
Investigation and Diagnosis
Tetanus can be diagnosed through the symptoms. But along with symptomatic diagnosis, a spatula test is used to confirm the diagnosis.
Spatula test: It involves inserting a spatula into the back of the throat. In case of no infection, the spatula will cause a gag reflex and the patient will try to push the spatula out of the mouth. But if the infection is positive then the spatula will cause the throat muscle to spasm and bite down onto the spatula.
Management
There are two types of treatment for tetanus:
Preventive treatment
- For people who are assumed to be completely or partially vaccinated against tetanus and who have an injury that makes them susceptible to a tetanus infection. A medication called tetanus immunoglobulin (TIG) is recommended if it has a tetanus-prone wound and there is a high risk that it could be contaminated by tetanus bacteria.2
Symptomatic treatment:
For people who have shown the symptoms of an active tetanus infection. Three main types of medication are used to overcome the symptoms of tetanus:1. Sedatives,2. Muscle Relaxants and3. Neuromuscular blocking agents.
Latest observations:
For vaccine application aldehyde (formaldehyde) detoxification is used to covert toxin into toxoids. It was observed that when formaldehyde was induced in tetanus toxin then out of the 1315 amino acids 41 were modified, of which 5 repeated modifications were observed in lysine residue of tetanus toxoid.19 This finding could be a milestone in the identification of specific amino acid responsible for the toxicity and target specific approaches. Adequate sedation is one of the possible treatments to prevent the severity of tetanus toxins.20 In recent years, the studies underlining the mechanism of neuraxial blocks in controlling sympathetic overactivity is been elucidated. Since the major cause of death is circulatory collapse, yet the mechanism of action is unclear and it is predicted that this might be because of altered myocardial functions that affect the catecholamine levels.
Prevention
Tetanus can be prevented by vaccinating with tetanus toxoid (Table-1). There are four combination vaccines used to prevent tetanus: DTaP (diphtheria, tetanus, and pertussis) and Tdap (tetanus, diphtheria, and pertussis) or Dt and Td. Two of these (DTaP and DT) are vaccinated to children younger than 7 years of age and two (Tdap and Td) are vaccinated to older children and adults. As recommended by the CDC for every ten years adults should receive a booster vaccine. Some of the most common myths are made clear in table-3. Further, this could be prevented as suggested in Figure 3.
Figure 3: Patient education and awareness
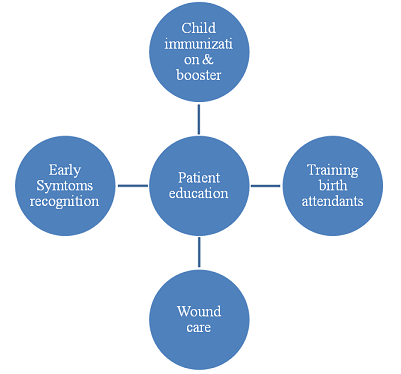
Table.2. Generic trade names of available vaccine/drugs for tetanus infection.
| Description |
Type |
Prescribed for |
| DPT |
Active immunization Vaccine |
Diphtheria, tetanus and pertussis (whooping cough) |
| Haemophilus B Conjugate |
Active immunization Vaccine for infants and children |
Haemophilus influenza type B, diphtheria, tetanus, and pertussis infections. |
| Pediarix Vaccine |
Immunization agent |
Diphtheria, tetanus, pertussis, hepatitis B and polio infections in infants and children. |
| Tdap |
Immunization agent |
Tetanus, diphtheria, and pertussis as a single dose in persons 11 to 64 years. |
| Tetanus Toxoid |
Immunization |
Tetanus |
Ayurvedic perspectives on treatment
Ayurvedic perspectives on the treatment of tetanus (based on probable correlation to Dhanustmbha):
In Ayurveda, the similar kind of signs and symptoms to tetanus are explained in the different context according to different authors and are specifically compared with different Vata vyadhis explained in Ayurveda, like Dhanurvata, Dhanustmbha, Antarayama (abhyantarayama), Bahirayama, etc. Dhanustambha was first described by Acharya Sushruta in the context of Vata vyadhi. While Acharya Charaka described it in two terminologies namely Antarayama and Bahirayama. According to Acharya vagbhata, it is explained in the context of Bahyayama (dhanushkamba, vegi). The disease is comparable to the tetanus of modern medicine.
Disease description:
Dhanustambha: It is caused when the vitiated vata affects the network of snayu (tendons/ligaments) making the body bent like a bow and hence the name. It is of two types namely Abhyantarayama and Bahyayama. Vitiated vata affects the snayu located in the toes, heels, abdomen, chest, and throat leads to muscular spasm, fixed gaze, lockjaw, rib fractures, kapha Vamana (vomiting) and inward bending of the body is Abhyantarayama (emprosthotonos). Vitiated Vata affects the external ligaments by which the body bends outwards like a bow is Bahyayama (opisthotonos) [Ref: su.s.ni 1].
Antarayama: It is the vata dosha which gets aggravated throughout the body and finally lodges in manya pradesha (carotid region) resulting in inward bending of the neck. It is associated with stiffness in manya pradesha and greeva (neck). Further, it is characterized by clenching of teeth, excessive salivation, stiffness from head to lower back and rigidity of face [Ref: c.s.chi.28/43-45]. Greevashritha dhamani are affected [Ref: a.h.ni.15/22-23].
Bahirayama: It is caused due to vata dosha that aggravates in greeva (backside of neck) causing constriction of siras (external vessel) which leads to bending of the jaw backward like a bow, the head moves towards back, the neck becomes rigid and squeezed, teeth are clenched along with yawning and excessive salivation. There is aphasia and chest is protruded [Ref: c.s.chi.28/45-48]. Excessive sweating, discolouration of teeth and face. It is Bahyayama, Dhanushkamba, vegi [Ref: a.h.ni.15/24-26].
According to Yogarathnakara, two contexts i.e., namely Dhanurvata and Dhanustambha have been mentioned which is caused because of vitiated vata associated with Kapha affecting the Dhamanis (vessels) leading to the stiffness, bending of the body like a bow hence referred as Dhanustambha [yo.r.ni.vata vyadhi nidana pg-507 Vaidhya Shri Lakshmipathi Shastry, Chaukambha Prakashan, Varanasi, 2012]. The other conditions can also be considered based on the signs and symptoms like Dantapatanaka/Dandaka: this is a condition in which the hands, feet, head, back, and hip becomes rigid and the body becomes stiff and still, like a rod due to vitiation of vata dosha [ref: c.s.chi28/51]. Abhighataja: could be considered as traumatic. The signs and symptoms similar to Bahirayama are also seen in the shava graha peeditha lakshana. [Ref: a.s.u.3/23]
Complications:
If the condition persists and leads to the fracture of the lumbar, spine, thigh; which is untreatable. [Ref: su.s.ni.1/57]. Patients with the following signs like decoloration of the face, closed mouth, wasting of muscles, loss of consciousness, profuse sweating, will die within 10 days. [yo.r.ni. vatavyadhi nidana]
Treatment:
Dhanustambha is said to be asadhya (untreatable) disease as per Ayurveda (c.s.chi-28/su.Ni-1). Based on the signs and symptoms, the treatment protocols are being employed. Snehana (oleation), Swedana (sudation), Basthi (Enema - with medicated oils, etc.), Nasya (Nasal drops), and Paana (oral medication). In Bahyayama and Abhyantarayama Sneha karma, sweda karma and Guggulu sevana is advised. [Ref: yo.r.ni. vatavyadhi nidana]
The treatment guidelines of Ardita Roga could be followed [Bharapraksha madhyama Khandha 24/186].
In every disorder, treatment follows a particular step which depends on location, dushya, etc. Ghee, oil, fat, and marrow are used and ingested, massage, enema, unctuous fomentations, wind-free place, wrappers, meat soups, mild, sweet-sour and salty edibles, whatever is bulk promoting is used on the patients of Vatika disorder [ch.s.chi.ch-28]. Oil cooked with an equal quantity of the juice taken out of the root and leaves of Nirgundi (Vitex negundo) vatika disorders. Oil cooked in a decoction of Karpasa seeds and horse gram also alleviates vata. [ch.s.chi.ch-28]. It is also found that; Nirgundi extract (juice) with honey thrice a day effectively cures tetanus. Chandra shekhara rasa (60-120 mg) mixed mother’s milk or Madhu (honey). Lakshmi Narayana rasa (30-60 mg) with adraka swarasa or madhu (honey) [Ref: textbook of kaumarabhritya pg: 598-599, ayodhya prasad achal, chaukambha surabharathi prakashan 2009].
Future prospects
Thought the bacterium Clostridium tetani is being studied for more than a century but still the mechanism has not been thoroughly understood. The practice of prevention is prevalent rather than treatment which is a cause of concern. Initial studies have been performed on the tetanus toxic protein by identifying the amino acids involved but the toxicity is not clear which is an area to explore and to come up with a solution. If the main amino acid constituents of toxin can be identified then the disease can be treatable at any stage of the infection. In conclusion, more awareness and care has to be taken in order to prevent tetanus. Climatic changes also aid to bacterial growth and production. The studies have to be widened which can cover the low-income countries which don’t have proper mass immunization. Farmers who are always exposed to soil need to have frequent monitoring of the disease. If tetanus is identified early then it is curable so “prevention is better than cure”.
Complications and myths involved with tetanus:
The major complications are due to the self-medication and high use of non-steroidal anti-inflammatory drugs (NSAID). The misconception is also because of various myths associated with the layman. A few are mentioned in table 3.
Table 3: Popular myths and its reasons
| Myths |
Inference |
Reason |
| Can get tetanus from rusty nails |
False |
It can be transmitted only if the bacteria is present |
| Tetanus shot won’t help if already been cut or bitten |
False |
The spore takes time for germination |
| If puncture wound bleeds a lot no need for tetanus shot |
False |
Wounds does not flush out all the tetanus spores. |
| Tetanus is a mild disease |
False |
In generalized tetanus the death rate is about 10-20% |
| There are easy and non toxic ways to prevent tetanus |
True |
By using vaccines |