
Patient Education
What is pneumonia?
“Pneumonia” is a Greek word meaning “inflammation of the lungs.” This illness is frequently acquired from exposure in the community and is therefore called community-associated pneumonia (CAP). It is an infection of the lungs caused due to either virus or bacteria. Rarely pneumonia can be caused by germs that cause tuberculosis (TB) or by fungi.
How common is pneumonia in children?
Pneumonia is the number one killer of children around the world and is the cause of 18% of all childhood deaths. An estimated 1.3 million child deaths in 2011 occurred due to pneumonia. More than 99% of all pneumonia deaths occur in developing countries and over 50% of global pneumonia deaths occur in India. It is estimated that 3.7 lakh children die of pneumonia annually in India.
How does pneumonia occur in a child?
Germs causing pneumonia may reach the child’s lungs through different routes. Although the information on how childhood pneumonia occurs, it is widely believed that common bacterial germs causing pneumonia are often already present in a child’s nose or throat and are then inhaled into the lungs, causing infection. Germs may also spread through contaminated air droplets or may result from blood infections. During or shortly after birth, babies are at higher risk of developing pneumonia from coming into contact with organisms in the birth canal. These germs then lead to irritation and inflammation of the lungs leading to fluid filling up the lungs and pneumonia.
Which are the germs that cause pneumonia?
Traditionally, viruses have been considered to be the most common cause of pneumonia in children between 1 and 36 months of age. In a recent study of acute pneumonia in hospitalized children between 2 months to 17 years of age, bacteria were identified in 60%, viruses in 45%, and mixed bacterial-viral infections in 23% of the cases. Common viruses causing pneumonia are influenza virus, parainfluenza virus, adenovirus, and respiratory syncytial virus. In children less than 5 years of age, the common bacteria causing pneumonia are H.influenzae, Streptococcus pneumonia, and staphylococcus aureus. Less common are Mycoplasma and Chlamydia pneumonia. In children more than 5 years of age, they have a higher rate of Mycoplasma infection. Streptococcus pneumoniae is the commonest cause of acute bacterial pneumonia in children. Other rare organisms causing pneumonia in older children are staphylococcus aureus.
How to distinguish between viral and bacterial pneumonia?
It is imperative to distinguish between viral pneumonia and bacterial pneumonia as there is no need to treat with antibiotics in viral pneumonia.
Viral pneumonia has a gradual onset. There is preceding cold, cough, low-grade fever, and decreased appetite in the patient or family members. Then there is an increase in irritability, respiratory congestion, cough, post-cough vomiting, and fever. The patient however is playful and not toxic. The doctor on examination may find the chest congested in both the lungs. There may be associated with wheezing.
Bacterial pneumonia on the other hand is associated with abrupt onset of fever. The child will be ill-looking and not really wheezing. He may have chest pains and cough.
Mycoplasma pneumonia typically presents with fever. When fever subsides, the cough appears. The symptoms usually last for 7-10 days.
What are the clinical features of pneumonia?
A child with pneumonia has a fever, and a cough. On a longer duration, he/she will complain of shortness of breath and chest pain. This is due to oxygen not reaching the blood due to inflamed lungs. Most of the younger children cannot bring up their sputum (phlegm) and swallow it leading to sticky stools. Occasionally, they may vomit after a bout of coughing and the vomit may contain phlegm. Older children may cough out the sputum and it may be green, yellow, or rust-colored suggestive of a bacterial infection.
What are the danger signs of pneumonia?
A child with pneumonia usually has a fever and cough. The parents should keep a strong vigilance and get the child to the hospital if there are the following danger signs:
Danger signs of pneumonia:
- Fast breathing
- Difficulty in feeding
- Not taking and food or water orally
- Child is turning blue
- Persistent vomiting and not passing urine
What tests are done to identify pneumonia?
Chest X-rays and laboratory tests are used to confirm the presence of pneumonia, including the extent and location of the infection and its cause.
Role of Chest X-ray: Routine use of chest radiography does not change the clinical outcome or treatment decisions in most patients with community-acquired pneumonia who are treated on an out-patient basis. Chest radiography is necessary to confirm the presence and determine the location of pneumonia in the following patients:
- Those less than 12 months of age with acute pneumonia who are hospitalized or severely ill
- Those who have recurrent disease or chronic medical conditions
- Those who develop complications; and those in whom the diagnosis is uncertain.
Various X-ray changes in pneumonia
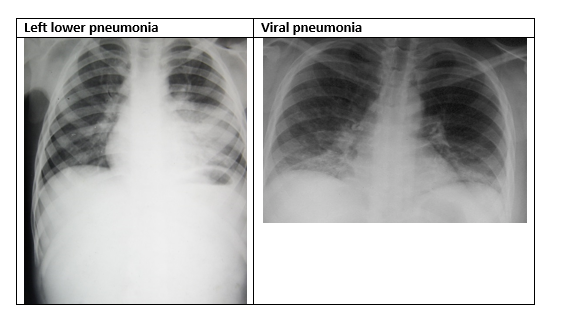
Among the various blood tests, your doctor may advise a hemogram (complete blood count) to check for increased white cell count, blood culture, and other biochemistries.
If a child is able to bring out sputum, the doctor may advise a sputum test also.
How to treat pneumonia?
After confirming the diagnosis of pneumonia and determining the extent and type of pneumonia, the doctor will prescribe medications. Mild pneumonia also is known as walking pneumonia does not require hospitalization and can be treated with oral medicines. For severe pneumonia leading to difficulty in breathing, hospitalization may be required and the child may require intravenous fluids, oxygen, and antibiotics.
In the case of bacterial pneumonia, the doctor will prescribe antibiotics. In the case of viral pneumonia, antibiotics are not required and medications to decrease congestion and fever such as cough syrups and paracetamol may be prescribed.
Taking rest and drinking plenty of fluids is always required in the management of pneumonia.
What should be the duration of antibiotics in patients with pneumonia?
Treatment courses of 10 days have been best studied, although shorter courses of 7 days may be just as effective, particularly for more mild disease managed on an outpatient basis. Infections caused by certain pathogens, notably community-acquired methicillin-resistant staphylococcus aureus (MRSA), may require longer treatment than those caused by S.pneumoniae.
How long does it take for recovery?
Most of the pneumonias recover within 7-10 days.
How to prevent pneumonia?
Since pneumonia can be caused by a variety of germs, one needs to avoid exposure to these germs. Washing hands with soap and water before you eat and after playing outside helps to kill most of the germs. Avoid smoking, have proper ventilation and sunlight in the house. Drink clean and filtered water preferably boiled water. Vaccination with Hib vaccine, Pneumococcal vaccine, and Influenza vaccine helps to prevent pneumonia due to Hemophilus influenza, pneumococcus and influenza virus respectively.
Which are the vaccines used to prevent pneumonia?
Pneumococcal vaccine:
Vaccination is the only available tool to prevent pneumococcal disease. There are over 90 types of S.pneumoniae bacteria. Originally the vaccine covered 7 commonest types causing pneumonia in children in the USA. The incidence of pneumococcal pneumonia due to vaccine serotypes has decreased substantially after the introduction of PCV-7 in the US children. Subsequently, now the vaccine covers 13 types of pneumococcus bacteria to cover the different types of pneumococci prevalent in different parts of the world especially the developing countries.
Dosing: Indian Academy of Pediatrics recommends 3 doses at 6, 10, and 14 weeks of age with a booster at 15 months. It is given intramuscularly.
- PCV13 is ideal & recommended routinely for all children 2-71 months of age and should be the vaccine of choice in India.
- In healthy children, 6 through 18 years of age due to their low risk of IPD, PCV13 is not recommended routinely. However, children with high-risk conditions are eligible for vaccination; get a single dose of PCV13.
- PCV13 vaccine is indicated for 19 years of age and older with immunocompromising conditions.
Hib vaccine:
With the widespread use of Hib vaccine worldwide and even in India as part of the National immunization program, pneumonia due to H. influenza b (Hib) is waning now.
Dosing: Indian Academy of Pediatrics recommends 3 doses at 6, 10, and 14 weeks of age with a booster at 15 months. It is given intramuscularly.
Influenza vaccine:
As per Indian Academy of Pediatrics (IAP) 2012, influenza vaccine is recommended for high risk children. High-risk children include those suffering from:
- Poor immunity including HIV infected children
- Asthma, heart disease, kidney disease, liver disease, diabetes mellitus, cerebral palsy
- Children on medicines that suppress immunity such as cancer chemotherapy or radiation therapy
- Patients with cancer
There are 2 types of influenza vaccines available. There is a vaccine that can be given as an injection (inactivated vaccine) and another one that can be given as a spray in the nose which is a live viral vaccine. The injectable vaccine is preferred in high-risk children, in pregnant women, and in children less than 2 years of age.
Dosing: For the first dose, in children, 2 years to less than 9 years of age, 2 doses of either the injectable or the nasal vaccine are given 1 month apart. In children above 9 years of age and adults, only a single dose is sufficient. Subsequently, the vaccine should be given every year. From 6 months to 2 years of age, the injectable vaccine is used as the live nasal vaccine is not recommended. Again in this age group, for the first time, 2 doses are recommended 1 month apart.